You are here: Eating Disorders/adults/MH/eating-disorders
If you're living with an eating disorder

Disclaimer - The information on this website is not absolute. It has been created by individuals who have experienced eating disorders and from their observations of their journey through recovery, so some of the text may not resonate with you. The information on this page may be triggering. If you need urgent mental health crisis support, call NHS111 Option 2.
Contents:
.
Warm words
Welcome to our page.
Are you currently facing challenges surrounding eating, your relationship with yourself and your body? This website has been put together by those who have experienced different eating challenges and recovered or in recovery. We want you to know you are not alone and support is available.
.
Words of encouragement
- You matter and your feelings are valid
- You are not the eating disorder; you are still yourself

- You are loved and will always be loved
- You have top-notch qualities, don’t forget about them
- Recovery is possible and there is life after an eating disorder. You can write down your reasons to recover
- Stay connected with your support network
- Reach out. You are worthy of help
- Talk to yourself as you would to someone you love
- There are times of joy beyond the eating disorder
- Each day is a new day
- Small steps are still progress
- Be proud of yourself for how far you have come
- You can still be a friend, partner, employee
- People will listen
- There is no one or reason to blame
- Find reasons to love yourself
- Small steps are still progress, celebrate them
- Every journey is different, but the end goal is the same
- Your eating disorder doesn’t have to fit in a specific box
- It’s ok to speak out, don’t be ashamed, your mind wants to silence you. You wouldn’t be ashamed of breaking your leg
- Forgive yourself
.bBack to top/menu
Explaining eating disorders
‘An eating disorder is a mental health condition where you use the control of food to cope with feelings and other situations. Anyone can get an eating disorder, but teenagers between 13 and 17 are mostly affected. With treatment, most people can recover from an eating disorder’ (NHS, 2021)
Click here for more information from the NHS explaining eating disorders.
Who could develop an eating disorder? Anyone, of any age, race, culture, gender, or ethnic background,

Types of Eating Disorders – Anorexia Nervosa, Bulimia Nervosa, Diabulimia, Binge Eating Disorder, Avoidant/Restrictive Food Intake Disorder (ARFID), Other Specified Feeding or Eating Disorder (OSFED) / Eating Disorders Not Otherwise Specified (EDNOS), Orthorexia, Rumination Disorder, Pica, Bigorexia.
Causes: Eating disorders are complex. There is no single reason. There can be a range of factors that could combine to make it more likely any one person could develop this condition.
Further explanations: Eating disorders are ever changing and different for everyone. Unhealthy eating behaviours may include but aren’t limited to eating too much or too little or worrying about your weight or body shape.
So many things can be going on at the same time and you can feel like things are so out of control.
You may feel the urge to want to put things in a box or label things you don’t understand, to normalise or minimise what you are experiencing.
Eating Disorders can become a crutch and feel like it is all you have got.
You do not have to focus on recovery if this feels like a long way off. Consider small more manageable steps to help you on the journey of recovery. Small steps are still steps.
Often there are religious holidays, festivals, rituals or periods of our lives that are focused on food. These can be difficult so don’t be afraid to ask for support.
Individual’s experience eating disorders and feelings differently. You could do certain behaviours or experience thoughts and activities that are unhealthy but make you feel good. It can be hard to let that go as that’s a coping mechanism.
Early habits - There can be early signs or habits that are unhealthy for individuals to do. It is a good idea to act quickly. Beat have a 'Know the first signs' poster which you can see to the right or you can download a copy here.
.Back to top/menu
Myths and truths
To view all of the myths please click here.+
- Mental illnesses, especially eating disorders are somewhat more ‘accepted’ now, more 'normal' and common. Still not everyone understands. It is an illness. You’d get treatment for a physical illness, so this is the same
- Individuals may feel alone as eating disorders are so specific and different for everyone. It can feel like others around you have it together and you don’t
- The reality of eating disorders being far from the stereotype. Anyone can have an eating disorder, for any reason. It is not about will power or self-control
- Myth - Eating disorders are about food and body image
Truth - It is often the complete opposite
- Myth - It’s your fault and is your decision
Truth - Cause can be varied. It is complicated. There are a variety of things that effect whether someone goes on to develop an eating disorder
- Myth – You must be a below a certain BMI to get help
Truth - BMI shouldn’t determine if you’re getting treatment or not, that isn’t the only way to measure at eating disorder
- Myth – It is just a phase and will pass
Truth - Don’t wait for yourself to get worse. – early intervention will help you recover
- Myth – I haven’t accessed help before so this will mean I won’t get support because I am not ill enough
Truth - It doesn’t matter if you’re going to your GP or anyone for help for the first time or have a long-term condition, you can get help
- Myth - You’ll have this forever
- Truth - You can recover
- Myth – All eating disorders are anorexia and are all about being skinny.
Truth - There is no standard eating disorder. People of all shapes and sizes can experience an eating disorder
- Myth - You have to be underweight to have an eating disorder. You can see if someone has an eating disorder by looking at them
Truth - Eating disorders are about more than food and weight. You can have an eating disorder at any weight or size. Eating disorders can’t always be seen. What you do see isn’t the whole picture. The issue is much deeper than food
- Myth- Eating disorders are a choice
Truth - Eating disorders are an illness. You can recover. There are so many things that contribute to an eating disorder, like biology/genetics, cultures, trauma
- Myth - Eating disorders only affect young girls
Truth - There is no standard eating disorder. It can happen to anybody of any age, gender identity, culture, and ability. BEAT say that in the UK there are around 1.25 million people who have an eating disorder. 25% of those affected by an eating disorder are male.
- Myth - Something or someone is to blame
Truth - Eating disorders happen for several reasons and are nobody’s fault. There can be lots of contributing factors, trauma, genetics, stress, biology, surroundings, psychology (core reasons)
- Myth - I will be like this forever
Truth - It may be in your life for now, however recovery is possible
.Back to top/menu
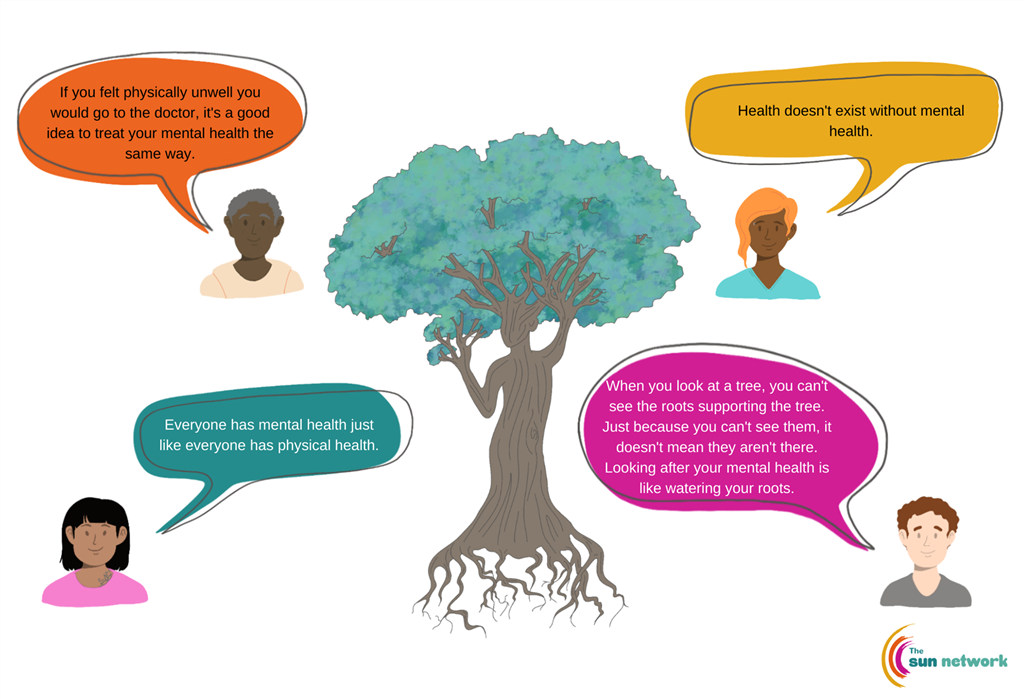
Physical health = Mental health
It is a common misconception that eating disorders are about physical looks. Whilst there are physical aspects such as weight loss or gain, bingeing, and vomiting, over or under eating, or over exercising, eating disorders are a mental health illness affecting thoughts and feelings. Physical and mental health are closely linked, and it is important to look after both.
Quiz
Back to top/menu
Signs and symptoms
Anyone can have an eating disorder; you don’t have to experience all symptoms to be struggling with one. Individuals who have their own experiences with eating disorders have put together a list of signs and symptoms to look out for, alongside a list of different eating disorders and their descriptions which you can view here.
.
How to start a conversation
Who to talk to.
When considering who to talk to about any concerns you might have with food, eating, your weight or shape, it is important to find someone you can trust and who can listen to you without judgement. This might be a teacher, a friend, a colleague, or a family member. You might also want to talk to a healthcare professional such as a GP. Choosing a time when you don't feel rushed can be important, and perhaps avoiding mealtimes or other potentially difficult times can be helpful too.
What to say? Helpful phrases and sentence starters+
- ‘I am struggling with…’
- ‘I am finding things hard …’
- ‘I think I need help…’
- ‘I am worried that I am not coping, can I talk to you…’
- ‘Have you got some time for me to talk about something I’m going through…’
- ‘I am not feeling myself at the moment. Can I talk to you?’
- ‘…I’m actually not fine’ – you don’t have too always be ok
You can ask someone to come to an appointment with you.
Helpful things to know:
- People may not understand or react how you’d hope or expect. Try not to let this put you off. Try someone else. Trust someone will listen
- Their reactions are about them and their understanding, it is not about you. It depends on their mental state and capacity at the time but does not mean they will never understand, listen or be there
.Back to top/menu
What might happen if you ask for help?
We know that speaking about this topic with healthcare professionals might seem overwhelming. We want to share some pointers as to what might happen at your appointments.
- Trust yourself at the GP surgery. You can have a say in your appointment. If your GP suggests you’re fine and you know you are not, don’t take no for an answer, you can ask at the reception to see another doctor/a doctor that is good with mental health. It is also ok to take someone with you to support you. You can also write down specific points you want to say
- Professionals will want to check your health. They need to get a clear understanding about your physical wellbeing to view you in a holistic way (all aspects of your whole self). Some may take blood tests, ECG’s, (recording of your heart activity) blood pressure, and weigh you. You can ask for this to not be shared with you if you choose, and you don’t have to look while they do these tests
- You may be referred to other services and specialists, and you may go on waiting lists. This may mean you could come across different professionals and specialists in your journey such as counsellors or therapists, specialist eating disorder staff, mental health staff, social workers, health care assistants, nurses or psychologists/psychiatrists
- Try not to be put off by professionals if they do not understand or if your experience isn’t as positive as you had hoped. Sometimes the advice you get might not always work for you. Professionals do not always get it right first time. Please don’t let any of this put you off asking for other support
.Back to top/menu
Wellbeing tool kit
 Self-care
Self-care
- Breaking the cycle, if may be helpful to look at the cycle of change - Beat has helpful information on this that can be viewed here
- Look after your physical health. If you are physically unwell don’t avoid seeing a health care professional
- Basic self-care, like brushing your teeth or having a shower is important for your physical and mental health in helping you feel better. Try to set yourself small goals, like getting dressed and washing your face or accepting that you’re allowed to look after yourself
- Prioritise yourself, this includes giving yourself time to rest and sleep, self-acceptance and self-love

Healthy distractions
- Puzzles, games, reading a book, listening to some music, meditation, taking a bath, yoga, Pilates, tai-chi
- Put your favourite film, TV program or music on
- If your ways of coping include self-harming or inflicting pain on yourself, try less damaging alternatives such as pinging an elastic bands, writing on your skin or holding ice cubes. These physical distractions could help
- Volunteer/charity work – this can be a great way to boost your confidence and aid your recovery
 Connecting - Is there someone you can talk to?
Connecting - Is there someone you can talk to?
- Have a catch up with a friend or family member. Contact someone you trust, it doesn’t have to be a phone call, and you can talk about anything
- Beat have a helpfinder on their website to help you find support in your area
- Beat has helplines you can call which are open 365 days a year from 9am–8pm during the week, and 4pm–8pm on weekends and bank holidays and they also have online chatrooms, one-to-one online advice chat options, 'Blossom' - which is an online structured group to help support those who are managing their eating disorder whilst waiting for NHS treatment and 'Invicta' - which is an online unstructured chat group where others with similar experiences can share helpful advice for recovery and their experiences, the chat room is moderated by BEAT employees so posts are approved before being 'published' to the group to ensure no posts are triggering or inappropriate
 Mindful- Find what works for you — gratitude, appreciating the little things
Mindful- Find what works for you — gratitude, appreciating the little things
- Try to step back and reflect on what is going on for you right now. You might find it helpful to write this down
- Get some fresh air. Take in your surroundings—connect with nature
- Writing down things to look forward to, reasons to recover
 Get creative — journal, scrapbook, write down your reasons to recover, paint, draw, crochet, or knit
Get creative — journal, scrapbook, write down your reasons to recover, paint, draw, crochet, or knit
- Write down your own positive affirmations and gratitude. You can do this on post-it notes, in a journal or on your phone
- Doing things that make you happy
Use recommended sites like NHS, Mind, BEAT, PEDS. Information can be damaging and unhealthy. Being aware of unhealthy sites that encourage negative behaviours/thoughts/actions. There can be negative and positive information online.
.Back to top/menu
Pandemic
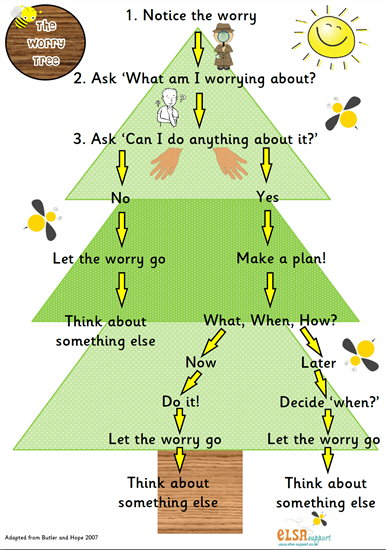 Coping with the change during the pandemic. It is a worrying time at the moment for many people, so anxieties are bound to be heightened, try and take things one step at a time (BEAT has information about shopping, routines and anxiety during the pandemic). You can write a worry list or worry tree here.
Coping with the change during the pandemic. It is a worrying time at the moment for many people, so anxieties are bound to be heightened, try and take things one step at a time (BEAT has information about shopping, routines and anxiety during the pandemic). You can write a worry list or worry tree here.
Beat has a section on their website with information on how to cope during the pandemic which you can view here.
- Being eligible for a vaccine. For information on vaccinations please click here
- Not wanting to get help with your physical and/or mental health challenges because of the effect the pandemic has had. Your wellbeing is important so you should still seek help, click here to go to view resources available to support you
- You might not initially see a medical professional face to face due to the pandemic, however you might get a phone or video call. This may change depending on the restrictions in place at the time you make contact
- Worrying about life post pandemic and social interactions can be triggering. Try not to rush yourself, trust how you are feeling and be kind to yourself when you are entering a difficult situation. Perhaps you could speak to a friend about your worries to set some goals for yourself. Try not to feel that as lockdown is easing you have to say yes to making plans or going out, you can say no if you don’t feel ready. You can make plans within the limits that you feel comfortable with
- Routines and rules changing can be disturbing. Setting yourself a healthy routine to provide some structure to your time can be useful
- You may be concerned about shopping. It could help you to make a shopping list for the items you need or want to buy. You can go shopping at quieter times in the day depending on opening hours (between 7am-9am and 7pm-9pm)
- Campaigns, advice and social media messages can be overwhelming. Advice and information from the government and other organisations are blanket messages that do not cover individual aspects of health. They aren’t always relevant to everyone and often can miss important aspects. Take a break from the news, you don’t have to engage with everything all the time
- Whether there is a pandemic or not you are worthy of help and there is support. It just might look different
- The pandemic will not last forever
- Pressure of being encouraged to exercise, socialise and ‘be happy’ because everything is returning to normal. This can be hard to manage and work through so be kind to yourself and focus on your mental wellbeing
.Back to top/menu
Support information
There is appropriate support and help for what you are going through.
Things you can do to make it easier for you when/with getting help:
- Ask someone to come to an appointment with you
- Making notes/plan of what you want to say
- Plan something nice after your appointment
- Choose a time and a place you are comfortable with
- Take it slow – you do not have to say it all in one appointment. Remember it is the start of a conversation and what’s important is getting it out in the open
What to do if you are unhappy with the service you access/can’t access:
- Firstly, you could speak to the service themselves through their complaints process. Don’t worry, this won’t prevent you from accessing further services if you require them
- If you wish not to speak to the service yourself, you are welcome to contact The SUN Network or you could go to Patient Advice and Liaison Service (PALS)
- There are a variety of other support services out there so if the one you are currently with isn’t working for you don’t worry
While you wait:
You could have been: referred and are on a waiting list, moving out of/into areas, moving back to home after being away, moving into community, inpatient or outpatient services or you could be between children and adult services and waiting to get support.
- Monitored chat rooms – Beat has helplines you can call which are open 365 days a year from 9am–8pm during the week, and 4pm–8pm on weekends and bank holidays and they also have online chatrooms, one-to-one online advice chat options, 'Blossom' - which is an online structured group to help support those who are managing their eating disorder whilst waiting for NHS treatment and 'Invicta' - which is an online unstructured chat group where others with similar experiences can share helpful advice for recovery and their experiences, the chat room is moderated by BEAT employees so posts are approved before being 'published' to the group to ensure no posts are triggering or inappropriate
- Self-care
- You can speak to your GP. They can help in different ways, they may offer to sign you off work
- Occupational support may be offered
- There are private healthcare avenues available
- You could access other local voluntary sector organisations
- There are helplines available to call
.Back to top/menu
Services (what is on offer)
- Support groups - PEDS and BEAT have support groups. These can be accessed through self-referrals, GP referrals and online portals. Due to the limited amount of support groups available, they can be at times difficult to access. There are however other support services you can go to and other resources you may find useful
- Support services - Keep Your Head has a list of support services for mental health and wellbeing
- The SUN Network co-produced some information leaflets, with the help of carers of loved ones with eating disorders and individuals who had lived experience of an eating disorder. The two free information leaflets can be accessed via this link and a leaflet about medical monitoring with eating disorders can be read and download here
- School/college/uni
- NHS - Cambridgeshire and Peterborough Foundation Trust (CPFT) Eating disorder services. CPFT run the Eating Disorder Service locally. Most people will be seen as outpatients, with a small number requiring a hospital inpatient stay. To access support for an eating disorder, please visit your GP.
- CPFT's Keeping Safe Programme - The Keeping Safe programme is the first step in your treatment. It has been developed to provide information to help you begin to make sense of your difficulties and to encourage you to take steps to minimise any potentially harmful effects caused by your eating disorder whilst you are waiting for treatment. The aims of the Keeping Safe programme are:
- to provide information about eating disorders
- to promote a better understanding of the effects of eating disorders
- to give guidance and harm minimization tips to help you keep yourself safe whilst you are waiting for treatment
- Primary Care Mental Health Service (PCMHS) - is a service that covers all surgeries in Cambridgeshire and Peterborough. The service provides specialist mental health support for GP surgeries so that patients with mental ill health can access prompt advice and support, receive help in a community setting and experience a more joined-up approach to care.
- Your GP surgery
- Beat have a helpfinder on their website to help you find support in your area
Voluntary organisations:
 Personalised Eating Disorder Support - PEDS - (Self-Refer) - offers assessment and support with signposting and where appropriate to service users, families and loved ones and professionals. We offer our service users individual sessions which are tailored to meet the unique needs of each person. We also provide family sessions which include practical help, education and support. We operate mostly remotely and sessions are via Microsoft Teams or Zoom. This includes assessments, 1:1s and groups (service users and carers). Face-to-face sessions, if required, are held at Boroughbury Medical Centre
Personalised Eating Disorder Support - PEDS - (Self-Refer) - offers assessment and support with signposting and where appropriate to service users, families and loved ones and professionals. We offer our service users individual sessions which are tailored to meet the unique needs of each person. We also provide family sessions which include practical help, education and support. We operate mostly remotely and sessions are via Microsoft Teams or Zoom. This includes assessments, 1:1s and groups (service users and carers). Face-to-face sessions, if required, are held at Boroughbury Medical Centre CPSL MIND is a mental health charity which promotes positive wellbeing across our communities and supports people on their road to recovery from a wide range of mental health challenges. They offer online support, community initiatives to connect people, counselling, Cognitive Behavioural Therapy, peer support groups, Perinatal services and opportunities to get involved with training, volunteering, campaigning and fundraising
CPSL MIND is a mental health charity which promotes positive wellbeing across our communities and supports people on their road to recovery from a wide range of mental health challenges. They offer online support, community initiatives to connect people, counselling, Cognitive Behavioural Therapy, peer support groups, Perinatal services and opportunities to get involved with training, volunteering, campaigning and fundraising Centre 33 — exists to help every young person in Cambridgeshire fulfil their potential and overcome problems through a range of free and confidential services - including housing, sexual health, family problems, and bullying
Centre 33 — exists to help every young person in Cambridgeshire fulfil their potential and overcome problems through a range of free and confidential services - including housing, sexual health, family problems, and bullying Lifecraft is a user-led organisation for adults in Cambridgeshire and Peterborough who experience mental health difficulties. They offer a range of free mental health services to help and support individuals in their wellbeing and recovery
Lifecraft is a user-led organisation for adults in Cambridgeshire and Peterborough who experience mental health difficulties. They offer a range of free mental health services to help and support individuals in their wellbeing and recovery Illuminate is an organisation specialising in mental health coaching and training to help make positive changes
Illuminate is an organisation specialising in mental health coaching and training to help make positive changes Beat – Beat provides Helplines for people of all ages, offering support and information about eating disorders no matter where you are in your journey. These Helplines are free to call from all phones.
Beat – Beat provides Helplines for people of all ages, offering support and information about eating disorders no matter where you are in your journey. These Helplines are free to call from all phones.
Our Helplines are open 365 days a year from 1pm – 9pm during the week, and 5pm–9pm on weekends and bank holidays. Support on the Helpline is available by phone, email, webchat (live link) through our social media accounts and by letter. Calls to the helpline are free from landlines and mobile phones within the UK and do not appear on itemised bills.
Sometimes our lines are busy. If you can't get through immediately, please do try again or try our one-to-one web chat or send us an email.
If you are in need of urgent help or medical advice for yourself or someone else, please contact 999 or the Samaritans on 116 123 if you or someone else is in immediate danger. If you are looking for medical advice, contact your GP or 111.
Helpline for England: 0808 801 0677
Helpline for Scotland: 0808 801 0432
Helpline for Wales: 0808 801 0433
Helpline for Northern Ireland: 08088 010 434
 SEED – (Support and Empathy for people with Eating Disorders) are a voluntary organisation and registered charity whom have first-hand experience of eating disorders and make a different to others who are challenged with this illness
SEED – (Support and Empathy for people with Eating Disorders) are a voluntary organisation and registered charity whom have first-hand experience of eating disorders and make a different to others who are challenged with this illness
.Back to top/menu
Resources
Books: Authors of lived experience and carer books:

- Hope Virgo
- Emma scrivener
- Jenny Langley
- Tina McGuff
- The Invisible Man - A Self-help Guide for Men With Eating Disorders, Compulsive Exercise and Bigorexia
- Samuel Pollen - author of The Year I Didn’t Eat
- Christopher Eccleston - I Love the Bones of You
- Rhik Samadder - I Never Said I Loved You
- Andrew Walen - Man Up to Eating Disorders
- MaleVoiced - this website is specifically for male ED suffers and has some brilliant resources including this great list of books
- Beat have suggested books
- Mindful Eating: A guide to rediscovering a healthy and joyful relationship with food - By Jan Chozen Bays
- Life without ED by Jenni Schaefer
- 8 keys to recovery by Geneen Roth
- The Inside Scoop on eating disorder recovery: Advice from two therapists who have been there by Colleen Reichmann and Jennifer Rollin
- Goodbye ED, Hello Me: Recover from your eating disorder and fall in love with life by Jenni Schaefer
- Body Image Workbook
- The secret language of eating disorders, Peggy Claude-Pierre
- The War of art - Steven Pressfield
- Sick enough: A guide to the medical complications of eating disorders by Jennifer L Gaudiani
-
Thinsanity by Glen Mackintosh
- Janet Treasure books - aimed at carers
Podcasts:
Apps:
Websites:

There are resources for carers which can be viewed here.
.
Helplines:

- Lifeline - 11am-11pm every day 0808 808 2121
- NHS First Response Service. In a mental health crisis? Call NHS 111 option 2
- Samaritans - 24hours a day, 365 days a year. Free line 116 123
- Beat (Adults) - Call for eating disorder support - 0808 801 0677
- Beat (Student Line) - 0808 801 0811
- Beat (Under 18's) - 0808 801 0711
- SEED Advice Line - (01482) 718130
- National Centre for Eating Disorders - 0845 838 2040
- Your GP surgery

